Researchers find a combination that reduces the plaques associated with the most common kind of dementia
Jessica Richburg
Perhaps all it takes is a little noise and an internal bubble bath to help drugs attack dementia. That is the oversimplified version of a study on Alzheimer’s – at least as seen in a mouse.
To make things a bit clearer: Australian scientists recently found a safer way to fight the disease using low-intensity ultrasound, microbubbles, and Aducanumab, an antibody treatment that targets the damaging amyloid plaques seen in Alzheimer’s. The ultrasound and microbubbles appeared to open the blood-brain barrier, a well-regulated system of blood vessels that work with immune and brain cells, thus letting in more of the drug. It also did something more…
So, what’s Alzheimer’s?
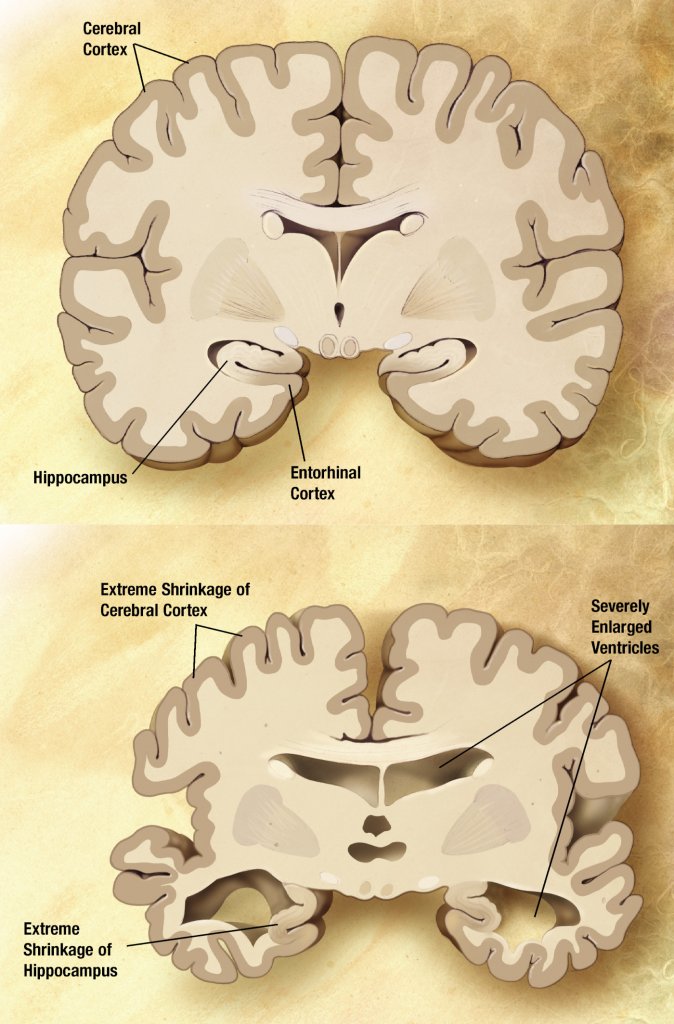
Alzheimer’s disease is a form of dementia (the loss of thinking skills) that causes brain cells to shrink and die. It is linked to the formation of the above-mentioned amyloid plaques, clumps of waste protein stuck together that appear to affect nerve function and longevity. Also seen are neurofibrillary tangles, a distorted form of a protein called tau that in its normal form helps maintain the cell’s shape.
Going by figures from 2016, roughly 44 million people worldwide suffer from Alzheimer’s and other forms of dementia – and Alzheimer’s is believed to make up 60-70% of them. But the nature of the disease means that the victims are not the only ones affected. Friends, family, and others also carry the burden.
In the early stages, plaque builds up in the hippocampus. This is a seahorse-shaped area of the brain important for us in memory, learning, thinking, finding directions, and more. Damage proceeds slowly enough that its victims can often feel themselves losing control of memories, thinking, and, ultimately, their bodies.
A curious thing
Gotz, of the Queensland Brain Institute in Australia, has been exploring Alzheimer’s treatment for decades, though his early work focused more on the neurofibrillary tangles. His work in ultrasound, however, started with a single question to himself in 2012.
“I was attending a conference in the first year after I had relocated from Sydney to Brisbane, and I was walking past a poster,” he told Truly Curious. “And I saw someone using ultrasound…. I thought, ‘Wouldn’t it be interesting to apply ultrasound to Alzheimer’s mice?’
“[The idea was] that in using ultrasound in combination with microbubbles, we could open the blood-brain barrier. Then, the amyloid that builds up in an Alzheimer’s patient – or in this case mouse – would be flushed out of the brain into the bloodstream.”
Ultrasound has been used in treatment against major tremors in Alzheimer’s and Parkinson’s patients. In fact, Gotz and his team were the first to show the benefits of ultrasound in Alzheimer’s. But the treatment was invasive, and used high-frequency ultrasound that dangerously overheated the target neurons.
So Gotz and two graduate students opted for a low-intensity ultrasound to clean out the amyloid plaque without boiling some neurons in the bargain.
Early steps
The early experiments did not go quite as planned. But the results were more interesting than expected. Rather than flushing the plaques into the bloodstream, opening the blood-brain barrier activated brain resident microglial cells. Once “awake,” these dormant microglial cells, the scavengers of the brain, digested the plaques and removed them.
Heartened, even though a little surprised, Gotz decided low-frequency ultrasound was the way to go – at least when dealing with Alzheimer’s in mice.
He had also had seen that ultrasound worked better if there were microbubbles in the blood to be agitated. So the team came up with a study that combined the effects of a combination of ultrasound, microbubbles and Aducanumab. The subjects were some hapless, genetically modified APP23 mice. These have a gene that produces the signature signs of Alzheimer’s, including those gunky plaques.

First, though, there were the microbubbles to make. For that, the team filled bubbles of phospholipid, the main component of cell membranes, with a non-toxic, non-flammable gas.
What gas?? Octafluoropropane, if you really want to know.
In the groups that called for it, the bubbles were activated and injected into the space behind the eye of the anesthetized mice.
The experiment
The APP23 mice were trained for five days to avoid shock in one section of a grid. If the mice quickly forgot the danger and got shocked again later, their memory was clearly not up to scratch. Apparently, a common problem with APP23 mice. Of course, remembering in general, and spatial memory in particular, relies a lot on the hippocampus, an at-risk area in Alzheimer’s.
Gotz and gang split the APP23 mice into multiple groups. One got no ultrasound, microbubbles or Aducanamab, the antibody treatment that targets the plaques. Another group got ultrasound and microbubbles but no Aducanamab. Yet another got just Aducanamab. The fourth was a combination of ultrasound, microbubbles and Aducanamab. They also got some wild-type rats to compare the lot to.

First, the four APP23 mice with the closest top scores in shock avoidance were distributed across the four groups. Then the four mice with the next highest scores were similarly distributed. And so forth.
The APP23 mice received nine treatments, with the groups getting a dose of fluorescent Aducanamab on the last day. They were tested for shock avoidance on the fourth day of treatment, and three days after the treatment was over.
Thereafter, they took brain samples to see how the treatments had affected the growth of plaques in different parts of the brain.
A few surprises
The researchers found that, by themselves, both ultrasound with microbubbles, and Acucanamab, were linked to fewer amyloid plaques in the hippocampus. In the cortex, though, it took all of them working together to clear out more plaques.
Initially, the scientists were gratified that that their low-intensity ultrasound did not cause heat damage.
There was, however, one surprising result.
Gotz had guessed that microbubbles opened up the blood-brain barrier, permitting the removal of amyloid plaques causing memory problems. But there was a wrinkle: Ultrasound with microbubbles seemed to improve memory function, even without removing amyloid plaques. Since opening up the blood-brain barrier opens the brain to attack, it helped to know that it need not be opened.
“We had assumed that you had to remove the amyloid to restore memory functions,” Gotz says.
Now researchers on the other side of Australia, at Curtin University, say they may have found the origin of the plaques – fat-carrying proteins leaking into the brain from blood vessels. And a PLOS Biology study suggests the plaques may originate in the liver.
The competition to beat Alzheimer’s is beating up. It doesn’t matter who gets there first. Either way, the world wins.
Jessica Richburg is a certified high school technical writing and grammar teacher with a degree in English.